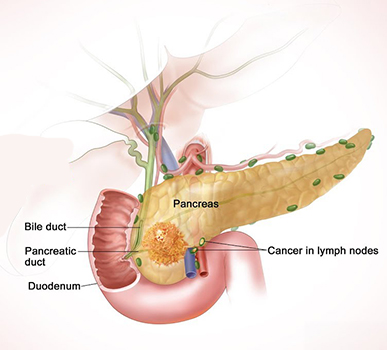
What Is a Pancreatic Neuroendocrine Tumor?
Pancreatic neuroendocrine tumors (NETs), or islet cell tumors, are a type of cancer that starts in the pancreas. (Cancer starts when cells in the body begin to grow out of control. Pancreatic NETs are a less common type of pancreatic cancer. Pancreatic neuroendocrine tumors start in neuroendocrine cells, a special kind of cell found in the pancreas. Neuroendocrine cells are also found in other areas of the body, but only cancers that form from neuroendocrine cells in the pancreas are called pancreatic neuroendocrine tumors. Neuroendocrine tumors start in the endocrine cells of the pancreas.
CAN-C known as one of the best centre for pancreatic neuroendocrine tumors treatment in Bangalore.
Here, you will find information about signs and symptoms, causes and risk factors, types, diagnosis, staging and prevention about neuroendocrine tumor.
Pancreatic NETs often release excess hormones into the bloodstream. Different types of tumors make different hormones, which can lead to different symptoms.
Gastrinomas: These tumors make gastrin, a hormone that tells the stomach to make more acid. Too much gastrin causes a condition known as Zollinger-Ellison syndrome, in which the stomach makes too much acid. This leads to stomach ulcers, pain, nausea, and loss of appetite, bleeding, anemia, feeling tired and being short of breath. If the bleeding is more severe, it can make stool black and tarry, diarrhea and weight loss.
Glucagonomas: These tumors make glucagon, a hormone that increases glucose (sugar) levels in the blood. Excess glucagon can raise blood sugar, sometimes leading to diabetes. This can cause symptoms such as feeling thirsty and hungry, and having to urinate often. Also symptoms such as diarrhea, weight loss, and malnutrition, and irritation of the tongue and the corners of the mouth. Most often a rash called necrolytic migratory erythema.
Insulinomas: These tumors make insulin, which lowers blood glucose levels. Too much insulin leads to low blood sugar, which can cause symptoms like weakness, confusion, sweating, and rapid heartbeat, passing out or even going into a coma, and having seizures.
Somatostatinomas: These tumors make somatostatin, which helps regulate other hormones. Symptoms of this type of tumor can include belly pain, nausea, poor appetite, weight loss, diarrhea, symptoms of diabetes (feeling thirsty and hungry, and having to urinate often), and jaundice (yellowing of the skin and eyes).
VIPomas: These tumors make a substance called vasoactive intestinal peptide (VIP). Too much VIP can lead to problems with diarrhea. Other symptoms can include nausea, vomiting, muscle cramps, feeling weak or tired, and flushing. People with these tumors also tend to have low levels of acid in their stomachs, which can lead to problems digesting food.
Carcinoid tumors: These tumors often make serotonin or its precursor, 5-HTP. Symptoms include flushing, diarrhea, wheezing, and a rapid heart rate. Over a long time, the hormone-like substances released by these tumors can damage heart valves, causing shortness of breath, weakness, and a heart murmur (an abnormal heart sound).
Non-functioning neuroendocrine tumors: Symptoms can be like those from exocrine pancreas cancers, including jaundice (yellowing of the eyes and skin), belly pain, and weight loss, liver enlargement, pain and loss of appetite. It can also affect liver function, sometimes leading to jaundice (yellowing of the skin and eyes) and abnormal blood tests.
A risk factor is anything that increases your chance of getting a disease such as cancer. Different cancers have different risk factors. Several factors can affect a person's chance of getting a neuroendocrine tumor (NET) of the pancreas.
Smoking: Smoking is a risk factor for pancreatic NETs.
Alcohol: Heavy alcohol use can also lead to conditions such as chronic pancreatitis, which may increase pancreatic NET risk.
Family history: Pancreatic NETs seem to run in some families.
Inherited genetic syndromes: Pancreatic neuroendocrine tumors and cancers can also be caused by genetic syndromes, such as: Neurofibromatosis, type 1, which is caused by mutations in the NF1 gene, Multiple endocrine neoplasia, type I (MEN1), caused by mutations in the MEN1 gene, Von Hippel-Lindau (VHL) syndrome, which is caused by mutations in the VHL gene.
Diabetes: Pancreatic NETs are more common in people with diabetes. Most of the risk is found in people with type 2 diabetes. This type of diabetes most often starts in adulthood and is often related to being overweight or obese.
Chronic pancreatitis: Chronic pancreatitis, a long-term inflammation of the pancreas, is linked with an increased risk of pancreatic NETs
Being overweight or obese: Being overweight or obese could be a risk factor for pancreatic NET.
In Bangalore, we at CAN-C has team of specialists to provide the very best treatment for people with neuroendocrine tumors.
Types of pancreatic neuroendocrine tumors are:
Tumor grade:
Pancreatic neuroendocrine tumors (NETs) are classified by tumor grade, which describes how quickly the cancer is likely to grow and spread.
1. Grade 1 (also called low-grade or well-differentiated) neuroendocrine tumors have cells that look more like normal cells and are not multiplying quickly.
2. Grade 2 (also called intermediate-grade or moderately differentiated) tumors have features in between those of low- and high-grade tumors.
3. Grade 3 (also called high-grade or poorly differentiated) neuroendocrine tumors have cells that look very abnormal and are multiplying faster.
Cancers that are grade 1 or 2 are called pancreatic neuroendocrine tumors. These cancers tend to grow slowly and can possibly spread to other parts of the body.
Cancers that are grade 3 are called pancreatic neuroendocrine carcinomas (NECs). These cancers tend to grow and spread quickly and can spread to other parts of the body.
Tumor function:
Pancreatic NETs are also named based on whether they are functioning (making hormones that cause symptoms) or non-functioning (not making hormones).
Functioning NETs: About half of pancreatic NETs make hormones that are released into the blood and cause symptoms. These are called functioning NETs. Each one is named for the type of hormone the tumor cells make.
1. Insulinomas come from cells that make insulin.
2. Glucagonomas come from cells that make glucagon.
3. Gastrinomas come from cells that make gastrin.
4. Somatostatinomas come from cells that make somatostatin.
5. VIPomas come from cells that make vasoactive intestinal peptide (VIP).
6. ACTH-secreting tumors come from cells that make adrenocorticotropic hormone (ACTH).
Most (up to 70%) functioning NETs are insulinomas. The other types are much less common.
Non-functioning NETs: These tumors don't make enough excess hormones to cause symptoms. Because they don't make excess hormones that cause symptoms, they can often grow quite large before they're found. Symptoms that may occur when they grow to a large size include abdominal (belly) pain, lack of appetite, and weight loss.
Carcinoid tumors: These NETs are much more common in other parts of the digestive system, although rarely they can start in the pancreas. These tumors often make serotonin.
We are one of the leading centre for pancreatic neuroendocrine tumors treatment in Bangalore.
Certain signs and symptoms might suggest that a person could have a pancreatic neuroendocrine tumor (NET), but tests are needed to confirm the diagnosis. Tests for Pancreatic Neuroendocrine Tumor are:
Imaging tests:
a. Computed tomography (CT) scan: A CT scan uses x-rays taken from different angles, which are combined by a computer to make detailed pictures of the organs.
b. Magnetic resonance imaging (MRI): Like CT scans, MRI scans show detailed images of soft tissues in the body. But MRI scans use radio waves and strong magnets instead of x-rays.
c. MR cholangiopancreatography (MRCP): It is a special type of MRI scan, which can be used to look at the pancreatic and bile ducts.
d. Ultrasound: Ultrasound tests use sound waves to create images of organs such as the pancreas.
e. Abdominal ultrasound: For this test, a wand-shaped probe is moved over the skin of the abdomen. It gives off sound waves and detects the echoes as they bounce off organs.
f. Endoscopic ultrasound (EUS): This test uses an endoscope with a small ultrasound probe on the end.
g. Cholangiopancreatography: This is an imaging test that looks at the pancreatic ducts and bile ducts to see if they are blocked, narrowed, or dilated.
h. Endoscopic retrograde cholangiopancreatography (ERCP): For this test, an endoscope (a thin, flexible tube with a tiny video camera on the end) is passed down the throat, through the esophagus and stomach, and into the first part of the small intestine.
i. Magnetic resonance cholangiopancreatography (MRCP): This is a non-invasive way to look at the pancreatic and bile ducts using the same type of machine used for standard MRI scans.
j. Percutaneous transhepatic cholangiography (PTC)
k. Radionuclide scans
l. Positron emission tomography (PET) scan
m. Somatostatin receptor scintigraphy (SRS or OctreoScan)
Blood and urine tests: Several types of blood and urine tests can be used to help diagnose pancreatic NET.
Biopsy: In many cases, the only way to know for sure if a person has some type of pancreatic NET is to remove cells from the tumor and look at them in the lab, which is called a biopsy. Percutaneous (through the skin) biopsy, Endoscopic biopsy and Surgical biopsy are used.
After someone is diagnosed with a pancreatic neuroendocrine tumor (NET), it is necessary to figure out if it has spread, and if so, how far. This process is called staging. The stage of a cancer describes how much cancer is in the body.
The staging system most often used for pancreatic NETs is the TNM system, which is based on 3 key pieces of information:
The size and extent of the main tumor (T): How large is the tumor? Has it grown into nearby structures or organs?
The spread to nearby lymph nodes (N): Has the cancer spread to nearby lymph nodes?
The spread (metastasis) to distant sites (M): Has the cancer spread to distant organs? (The most common site of spread is the liver.)
We are the pancreatic neuroendocrine tumors treatment specialist centre in Bangalore.
There is no sure way to prevent pancreatic neuroendocrine tumors (NETs). But, there are things you can do that might lower your risk.
Do not smoke: Smoking is an avoidable risk factor for pancreatic NET. Quitting smoking may help lower risk.
Limit alcohol use: Heavy alcohol use has been linked to pancreatic NETs. Heavy alcohol use can lead to conditions such as chronic pancreatitis, which has been associated with an increased risk of pancreatic NET.
"CAN-C: Expertise in providing pancreatic neuroendocrine tumors treatment in Bangalore."
Make An Appointment Today
How Neuroendocrine Tumor is treated?
Two general types of surgery can be used for pancreatic neuroendocrine tumors (NETs):
a. Potentially curative surgery is used when the results of exams and tests suggest that it's possible to remove (resect) all the cancer.
Types of potentially curative surgery include enucleation (removing only the tumor), central pancreatectomy, distal pancreatectomy, the Whipple procedure (pancreaticoduodenectomy), and total pancreatectomy. The type of surgery needed depends on several factors, including the location, size, and specific kind of pancreatic NET (functioning or nonfunctioning).
b. Palliative surgery may be done if imaging tests show that the cancer is too widespread to be removed completely. This surgery is done to reduce tumor size to relieve symptoms from excess hormone production or to prevent certain complications like a blocked bile duct or intestine.
If the cancer has spread too far to be removed completely, any surgery being considered would be palliative (intended to relieve symptoms). This type of surgery may be considered in some people with pancreatic NETs whose tumor has recurred and is causing local problems or is making too many hormones that are causing symptoms.
Radiation therapy uses high-energy rays (such as x-rays) or radioactive particles to kill cancer cells. Surgery is the main treatment for most pancreatic neuroendocrine tumors (NETs), but radiation therapy may be an option for those who can't have surgery for some reason. It may also be given after surgery in some cases if there's a chance some of the tumor was not removed and is causing problems. Radiation is sometimes used to treat pancreatic NETs that have spread to the bone and are causing pain.
External beam radiation therapy: External beam radiation therapy uses a machine that delivers a beam of radiation to a specific part of the body. Before your treatment starts, the radiation team will determine the correct angles for aiming the radiation beams and the proper dose of radiation. The treatment is much like getting an x-ray, but the radiation is stronger. The procedure itself is painless.
Radioactive drugs: Radioembolization: It combines embolization with radiation therapy and can be used to treat liver metastases. Peptide receptor radionuclide therapy (PRRT): People with somatostatin receptor-positive neuroendocrine tumors may be candidates for PRRT.
We at CAN-C, provide excellent treatment (in Bangalore) for pancreatic neuroendocrine tumors using the latest techniques.
Chemotherapy (chemo) uses anti-cancer drugs injected into a vein or taken by mouth to kill cancer cells. These drugs enter the bloodstream and reach almost all areas of the body, making this treatment useful for some types of cancers that have spread.
Chemo is most often used to treat pancreatic neuroendocrine tumors (NETs) if they:
a. Have not responded to other medicines (such as somatostatin drugs or targeted therapy),
b. Have spread to other organs,
c. Are large or growing quickly,
d. Are causing severe symptoms, or
e. Are high grade
The most commonly used drugs for pancreatic NETs include: Doxorubicin (Adriamycin), Streptozocin, Fluorouracil (5-FU), Dacarbazine (DTIC), Temozolomide (Temodar), Capecitabine (Xeloda), Oxaliplatin (Eloxatin)
Some tumors might be treated with more than one drug. Possible combinations include: Doxorubicin plus streptozocin, 5-FU plus doxorubicin plus streptozocin, Temozolomide plus capecitabine, 5-FU plus streptozocin.
Targeted drugs work differently from standard chemo drugs. These drugs target specific parts of cancer cells.
The targeted drugs used to treat pancreatic neuroendocrine tumors (NETs) work by blocking angiogenesis (the growth of new blood vessels that nourish cancers) or important proteins (called tyrosine kinases) in cancer cells that help them grow and survive.
Sunitinib (Sutent): Sunitinib blocks several tyrosine kinases and attacks new blood vessel growth. It has been shown to help slow tumor growth.
Everolimus (Afinitor): Everolimus blocks a protein known as mTOR, which normally helps cells grow and divide. It has been shown to help treat advanced pancreatic NETs.
CAN-C: Top and outstanding cancer centre for pancreatic neuroendocrine tumors treatment in Bangalore.
Our Doctors
Dr. Dinesh M G
Specialty: Surgical Oncologist & Laparoscopic Oncosurgeon
Dr. Dinesh M G, is an efficient surgeon specialized in oncology committed to the care and improvement of quality of life of cancer patients. His exceptional surgical skills, teamwork and knowledge are laudable. He is skilled in performing various minimal access oncologic surgeries and has mastered complex open surgeries in the field of oncology.
Completing MBBS from KIMS, Bangalore followed by MS - General Surgery from JJM Medical College, Davangere and M. Ch - Surgical Oncology from Kidwai Memorial Institute of Oncology, he has a Fellowship in Minimal Access Oncology from Basavatarakam Indo American Cancer Institute.

