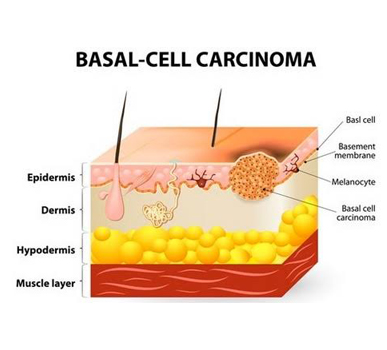
What is Basal Cell Cancer?
Basal cell cancer (also called basal cell carcinoma) is most common type of skin cancer. Basal cell carcinoma begins in the basal cells - a type of cell within the skin that produces new skin cells as old ones die off. These cancers start in the basal cell layer, which is the lower part of the epidermis. Basal cell cancers usually develop on areas exposed to the sun, especially the face, head, and neck, but they can occur anywhere on the body.
What causes basal cell skin cancers?
Most basal cell skin cancers are caused by repeated and unprotected skin exposure to ultraviolet (UV) rays from sunlight, as well as from man-made sources such as tanning beds. UV rays can damage the DNA inside skin cells. DNA is the chemical in each of our cells that makes up our genes, which control how our cells function.
We provide basal cell skin cancer treatment in Bangalore.
Here, you will find information about signs and symptoms, causes and risk factors, types, diagnosis, staging and prevention about basal cell cancer.
Symptoms of basal cell carcinomas are:
Flat, firm, pale or yellow areas, similar to a scar
Raised reddish patches that might be itchy
Small, pink or red, translucent, shiny, pearly bumps, which might have blue, brown, or black areas
Pink growths with raised edges and a lower area in their center, which might contain abnormal blood vessels spreading out like the spokes of a wheel
Open sores (which may have oozing or crusted areas) that don't heal, or that heal and then come back
CAN-C: Best centre in Bangalore for providing leading-edge treatment for basal cell skin cancer with the highest standard of care.
A risk factor is anything that raises your risk of getting a disease such as cancer. Different cancers have different risk factors. Still, it's important to know about the risk factors for basal cell skin cancer because there may be things you can do that could lower your risk of getting it.
Several risk factors make a person more likely to get basal cell skin cancer are:
Ultraviolet (UV) light exposure: Exposure to ultraviolet (UV) rays is thought to be the major risk factor for most skin cancers. Sunlight is the main source of UV rays. Tanning beds are another source of UV rays.
Having light-colored skin: Anyone can get skin cancer, but people with light-colored skin have a much higher risk than people with naturally darker skin color. This is because the skin pigment melanin has a protective effect in people with darker skin.
Albinism is an inherited lack of protective skin pigment: People with this condition may have pink-white skin and white hair. They have a very high risk of getting sunburns and skin cancer, so they need to be careful to protect their skin.
Being older: The risk of getting basal cell skin cancers rises as people get older. This is probably because of the buildup of sun exposure over time. But these cancers are becoming more common in younger people as well, probably because they are spending more time in the sun with their skin exposed.
Exposure to certain chemicals: Being exposed to large amounts of arsenic increases the risk of developing basal cell skin cancer. Arsenic is an element found naturally in well water in some areas. It's also used in making some pesticides and in some other industries.
Radiation exposure: People who have had radiation treatment have a higher risk of developing skin cancer in the area that received the treatment. This is particularly a concern in children who have had radiation treatment for cancer.
Previous skin cancer: People who have had a basal cell cancer have a much higher chance of developing another one.
Long-term or severe skin inflammation or injury: Scars from severe burns, areas of skin over serious bone infections, and skin damaged by some severe inflammatory skin diseases are more likely to develop skin cancers, although this risk is generally small.
Psoriasis treatment: Psoralens and ultraviolet light (PUVA) treatments given to some patients with psoriasis (a chronic inflammatory skin disease) can increase the risk of developing basal cell skin cancer and probably other skin cancers.
Xeroderma pigmentosum (XP): This very rare inherited condition reduces the ability of skin cells to repair DNA damage caused by sun exposure. People with this disorder often develop many skin cancers, starting in childhood.
Basal cell nevus syndrome (also known as nevoid basal cell carcinoma syndrome or Gorlin syndrome): In this rare congenital (present at birth) condition, people develop many basal cell cancers over their lifetime. People with this syndrome may also have abnormalities of the jaw (and other bones), eyes, and nervous tissue.
Weakened immune system: The immune system helps the body fight cancers of the skin and other organs. People with weakened immune systems (from certain diseases or medical treatments) are more likely to develop many types of skin cancer, including basal cell cancer, squamous cell cancer, melanoma, and less common types such as Kaposi sarcoma and Merkel cell carcinoma.
Human papillomavirus (HPV) infection: Human papillomaviruses (HPVs) are a group of viruses, many of which can cause papillomas, or warts. The warts that people commonly get on their hands and feet are not related to any form of cancer. But some HPV types, especially those that affect the genital and anal areas and the skin around the fingernails, seem to be related to skin cancers in these areas.
There are a number of different types of BCC. Each type can look and behave differently. They include:
Nodular basal cell skin cancer
Superficial basal cell skin cancer
Morphoeic basal cell skin cancer - also known as sclerosing or infiltrating basal cell skin cancer
Pigmented basal cell skin cancer
Basosqamous Carcinoma
It's very rare for basal cell skin cancer to spread to another part of the body to form a secondary cancer. It's possible to have more than one basal cell cancer at any one time and having had one does increase your risk of getting another.
We provide accurate treatment options for basal cell cancer treatment in Bangalore.
If you have an abnormal area that might be skin cancer, you need to undergo some tests to find out if it is cancer or some other skin condition. Some of the diagnosis tests includes:
Medical history and physical exam: Usually the first step is you will be asked about symptoms, such as when the mark first appeared on the skin, if it has changed in size or appearance, and if it has been painful, itchy, or bleeding.
Skin biopsy: If the doctor thinks that a suspicious area might be skin cancer, the area (or part of it) will be removed and sent to a lab to be looked at under a microscope. This is called a skin biopsy. If the biopsy removes the entire tumor, it's often enough to cure basal cell skin cancers without further treatment. There are different types of skin biopsies: Shave (tangential) biopsy, Punch biopsy, Excisional and incisional biopsies, Examining the biopsy samples
Lymph node biopsy: It isn't common for a basal cell cancer to spread beyond the skin, but if it does it usually goes first to nearby lymph nodes, which are bean-sized collections of immune cells. A lymph node biopsy may be done to find out if cancer has spread to them. Types: Fine needle aspiration (FNA) biopsy, Surgical (excisional) lymph node biopsy
Imaging tests: Spread of the cancer deeply below the skin or to other parts of the body is rare for basal cell cancers, so most people with one of these skin cancers don't need imaging tests. But if the cancer is spreading outside the skin, imaging tests such as MRI or CT scans of the area might be done.
After someone is diagnosed with cancer, it is necessary to figure out if it has spread, and if so, how far. This process is called staging. The stage of a cancer describes how much cancer is in the body. It helps determine how serious the cancer is and how best to treat it.
How is the stage determined?
The system most often used to stage basal cell skin cancers is the TNM system. It applies basal cell skin cancers of the head and neck area (lip, ear, face, scalp and neck). The stage is based on 3 key pieces of information:
The size of the tumor (T) and if it has grown deeper into nearby structures or tissues, such as a bone
If the cancer has spread to nearby lymph nodes (N)
If the cancer has spread (metastasized) to distant parts of the body (M)
We are well-known for providing most-effective basal cell carcinoma/cancer treatment in Bangalore.
There is no sure way to prevent all basal cell skin cancers. But there are things you can do that could lower your risk of getting basal cell cancer and other skin cancers.
Limit your exposure to ultraviolet (UV) rays: The most important way to lower your risk of basal cell skin cancers is to limit your exposure to UV rays. Practice sun safety when you are outdoors.
Avoid harmful chemicals: Exposure to certain chemicals, such as arsenic, can increase a person's risk of skin cancer. People can be exposed to arsenic from well water in some areas, pesticides and herbicides, some medicines and imported traditional herbal remedies, and in certain occupations (such as mining and smelting).
Check your skin regularly: Checking your skin regularly may help you spot any new growths or abnormal areas and show them to your doctor before they even have a chance to turn into skin cancer.
Avoid weakening your immune system (when possible): Having a weakened immune system increases your risk of getting skin cancer, and if you do get it, it might be harder to treat. Infection with HIV, the virus that causes AIDS, can weaken the immune system.
Medicines to lower risk: Some people at increased risk for skin cancer, such as people with certain inherited conditions or a weakened immune system, might be helped by medicines that could lower their risk (known as chemoprevention).
"CAN-C: Expert in rendering basal cell cancer treatment in Bangalore."
Make An Appointment Today
How Basal Cell Cancer is treated?
When detected early, most basal cell carcinomas (BCCs) can be treated and cured. The goal of treatment for basal cell carcinoma is to remove the cancer completely. Several types of treatment can be used to remove or destroy basal cell skin cancers. The options depend on factors such as the tumor size and location, and a person's age, general health, and preferences. All of the treatments listed here can be effective when used in appropriate situations.
Surgery is a common treatment for basal cell skin cancers. Different surgical techniques can be used. The options depend on the type of skin cancer, how large the cancer is, where it is on the body, and other factors. For skin cancers with a high risk of spreading, surgery sometimes will be followed by other treatments, such as radiation or chemotherapy.
1. Excision: This is similar to an excisional biopsy. For this procedure, the skin is first numbed with a local anesthetic. The tumor is then cut out with a surgical knife, along with some surrounding normal skin. Most often, the remaining skin is then carefully stitched back together. This type of surgery will leave a scar.
2. Curettage and electrodesiccation: In this treatment, the cancer will be removed by scraping it with a long, thin instrument with a sharp looped edge on one end (called a curette). The area is then treated with an electric needle (electrode) to destroy any remaining cancer cells. Curettage and electrodesiccation is a good treatment for superficial (confined to the top layer of skin) basal cell cancers. It will leave a scar.
3. Mohs surgery: Mohs surgery (also known as Mohs micrographic surgery, or MMS) is sometimes used when there is a high risk the skin cancer will come back after treatment, when the extent of the skin cancer is not known, or when the goal is to save as much healthy skin as possible, such as with cancers near the eye or other critical areas such as the central part of the face, the ears, or fingers.
4. Lymph node surgery: If lymph nodes near a basal cell skin cancer are enlarged, biopsy is needed to check for cancer cells. Sometimes, many nodes might be removed in a more extensive operation called a lymph node dissection. The nodes are then looked at under a microscope for signs of cancer. This type of operation is more extensive than surgery on the skin.
5. Skin grafting and reconstructive surgery: After surgery to remove a large basal cell skin cancer, it may not be possible to stretch the nearby skin enough to stitch the edges of the wound together. In these cases, healthy skin can be taken from another part of the body and grafted over the wound to help it heal and to restore the appearance of the affected area. Other reconstructive surgical procedures, such as moving 'flaps' of nearby skin over the wound, can also be helpful in some cases.
CAN-C: We provide best treatment for basal cell cancer (in Bangalore) at any stage of the disease.
Radiation therapy uses high-energy rays (such as x-rays) or particles (such as photons, electrons, or protons) to kill cancer cells.
When is radiation therapy used?
If a tumor is very large or is on an area of the skin that makes it hard to remove with surgery, radiation therapy may be used as the main treatment. Radiation therapy can also be useful for some patients who, for other health reasons, can't have surgery. Radiation therapy can often cure small basal cell skin cancers and can delay the growth of more advanced cancers.
Radiation is also useful when combined with other treatments. For example, radiation can be used after surgery as an adjuvant (additional) treatment to kill any small areas of remaining cancer cells that may not have been visible during surgery. This lowers the risk of cancer coming back after surgery. Radiation may also be used to help treat skin cancer that has spread to lymph nodes or other organs.
How is radiation therapy given?
When radiation therapy is used to treat skin cancers, the radiation is focused from outside the body onto the tumor. This is often done using a beam of low-energy x-rays (superficial radiation therapy) or electrons (electron beam radiation). These types of radiation don't go any deeper than the skin. This helps limit the side effects to other organs and body tissues.
Getting radiation treatment is much like getting an x-ray, but the radiation is stronger and aimed more precisely at the cancer. The procedure itself is painless.
Systemic chemotherapy (chemo) uses anti-cancer drugs that are injected into a vein or given by mouth. These drugs travel through the bloodstream to all parts of the body. Unlike topical chemotherapy, which is applied to the skin, systemic chemotherapy can attack cancer cells that have spread to lymph nodes and other organs.
If basal cell carcinoma has spread, chemo might be an option, although an immunotherapy drug might be used first. If chemo is used, drugs such as cisplatin and 5-fluorouracil (5-FU) might be options. These drugs are given into a vein (intravenously, or IV). They can often slow the spread of these cancers and relieve some symptoms. In some cases, they might shrink tumors enough so that other treatments such as surgery or radiation therapy can be used.
Basal cell carcinoma very rarely reaches an advanced stage, so systemic chemotherapy is not typically used to treat these cancers. Advanced basal cell cancers are more likely to be treated with targeted therapy.
We are recognized as a centre of excellence for basal cell cancer treatment (in Bangalore) with remarkable results.
These drugs target parts of skin cancer cells that make them different from normal skin cells. Targeted drugs work differently from standard chemotherapy drugs. They may work sometimes when chemotherapy drugs don't.
1. Hedgehog pathway inhibitors: Vismodegib (Erivedge) and sonidegib (Odomzo) are targeted drugs that can be used to treat some advanced or recurrent basal cell skin cancers. These drugs are capsules.
It's very rare for basal cell cancers to reach an advanced stage, but if they do, these cancers can be hard to treat. Most basal cell cancers have mutations (changes) in genes that are part of a cell signaling pathway called hedgehog. (Cell signaling pathways are how a cell gives instructions from one part of the cell to another, or to other cells.) The hedgehog pathway is crucial for the development of the embryo and fetus and is important in some adult cells, but it can be overactive in basal cell cancer cells, helping them grow. These drugs target a protein in this pathway.
For basal cell cancers that have spread or come back after surgery or other local treatments, these drugs have been shown to help shrink tumors in some people.
2. EGFR inhibitors: Basal cell skin cancer cells often have too much of a protein called EGFR on their surfaces, which can help them grow. Drugs that target this protein, such as cetuximab (Erbitux), have been used to shrink some of these cancers.
The immune system normally helps protect the body against germs, and it can also help destroy cancer cells. Immunotherapy is the use of medicines to stimulate a person's own immune system to recognize and destroy cancer cells more effectively. It can be used to treat some people with advanced basal cell skin cancer.
Immune checkpoint inhibitors: An important part of the immune system is its ability to keep itself from attacking normal cells. To do this, it uses "checkpoints", which are proteins on immune cells that need to be turned on (or off) to start an immune response. Cancer cells sometimes use these checkpoints to avoid being attacked by the immune system. But drugs that target checkpoint proteins, called checkpoint inhibitors, can help restore the immune response against cancer cells.
Cemiplimab (Libtayo): Cemiplimab (Libtayo) is a drug that targets PD-1, a checkpoint protein on T cells (a type of immune system cell) that normally helps keep these cells from attacking other cells in the body. By blocking PD-1, this drug boosts the immune response against cancer cells.
This drug can be used in people with advanced basal cell skin cancer that cannot be cured with surgery or radiation therapy. This drug is given as an intravenous (IV) infusion.
We at CAN-C are specialized in delivering high-quality basal cell cancer treatment in Bangalore.
